Male androgenetic alopecia (MAA) is the most common cause of hair loss in men, characterised by progressive follicular miniaturisation affecting the frontal scalp, temples and vertex. Histologically, MAA is associated with miniaturised hair follicles, sebaceous pseudohyperplasia, and increasing evidence of chronic low-grade micro-inflammation within the pilosebaceous unit. Recent genome-wide association studies have highlighted the complex and heterogeneous aetiology of MAA, identifying over 70 genetic risk loci spanning WNT signalling, immune pathways, melatonin signalling, and androgen and epidermal growth factor (EGF) pathways. Despite this complexity, current treatments remain limited, and combination therapeutic approaches are often required to optimise outcomes.
Topical ketoconazole is a widely available and inexpensive azole antifungal commonly used to treat dandruff and seborrhoeic dermatitis. Emerging clinical evidence suggests that ketoconazole may confer measurable benefits in MAA when used adjunctively. However, the biological mechanisms underpinning this effect remain poorly understood and whether its apparent benefits in MAA arise from direct effects on hair follicle epithelial biology, indirect immunomodulatory effects, microbiome-mediated mechanisms, or a combination of these factors.
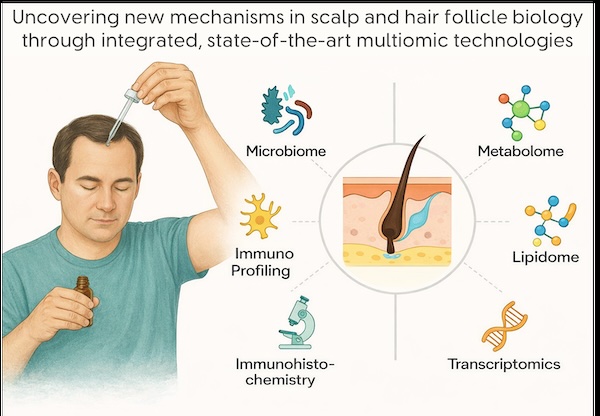
This PhD project aims to define how topical ketoconazole alters human scalp hair follicle biology in vivo, using an integrated multi-omics and tissue-level approach. A central hypothesis is that alterations in the scalp microbiome – particularly species such as Malassezia restricta – drive changes in inflammatory signalling within the hair follicle niche, contributing to disease progression, and that ketoconazole exerts therapeutic benefit by modulating this micro-environment.
The student will undertake a prospective, controlled clinical study of men with early-stage MAA, and examine the biological effects of ketoconazole. Analysis of swab samples will employ next-generation sequencing of the microbiome, metabolomic and lipidomic mass-spectrometry-based methods. Scalp tissue analysis will employ immunohistochemistry and transcriptomics analyses. By integrating these microbial, metabolic, lipid and cellular datasets, this project will generate novel mechanistic insights into the biology of MAA and the mode of action for the beneficial effects of a widely used topical therapy.
The findings have the potential to inform more rational combination treatments for MAA and has relevance to a rapidly growing area within dermo-cosmetics which is aligned with industry-facing translational skin research.
Representative Publications / References
https://pubmed.ncbi.nlm.nih.gov/31858672/ Fields, Jaime R et al. “Topical ketoconazole for the treatment of androgenetic alopecia: A systematic review.” Dermatologic therapy vol. 33,1 (2020): e13202. doi:10.1111/dth.13202
https://pubmed.ncbi.nlm.nih.gov/23496820/ Hosogaya, Naoki et al. “The heme-binding protein Dap1 links iron homeostasis to azole resistance via the P450 protein Erg11 in Candida glabrata.” FEMS yeast research vol. 13,4 (2013): 411-21. doi:10.1111/1567-1364.12043
https://pubmed.ncbi.nlm.nih.gov/16115827/ Pina-Vaz, Cidália et al. “Potent synergic effect between ibuprofen and azoles on Candida resulting from blockade of efflux pumps as determined by FUN-1 staining and flow cytometry.” The Journal of antimicrobial chemotherapy vol. 56,4 (2005): 678-85. doi:10.1093/jac/dki264